Rescue Rehab & Animal Osteopathy: Working Without a History
You’ve taken a thorough case history before. You know the questions to ask: previous injuries, surgical history, current medications, competition or working demands. You have a system, and it works well. Then a rescue animal walks through the door, and half the boxes on your intake form simply can’t be filled in.
This is one of the more clinically interesting challenges in animal osteopathy — and one that isn’t discussed anywhere near enough. Rescue animals, whether dogs, horses, or other species, present with histories that are incomplete by definition. The new owner may know a little. The rehoming organisation may know slightly more. But the first months, years, or even the formative developmental period of that animal’s life? Often a blank.
That blank is not just an administrative inconvenience. It has real clinical implications for how you approach assessment, how you interpret findings, and how you frame your treatment goals. Understanding those implications makes you a more effective practitioner — not just for rescue patients, but for any animal whose lived experience cannot be neatly documented.
Why the Missing History Changes Everything
In a standard presentation, history guides hypothesis. You know the horse had a fall six months ago; that informs where you look and what you expect to find. You know the dog had TPLO surgery on the left stifle two years back; compensation patterns downstream and upstream of that joint make immediate clinical sense.
With a rescue patient, you lose that interpretive scaffold. What you find on assessment has to stand more independently — but it also has to be held more lightly. A compensatory pattern that would normally point clearly to a known incident instead becomes a question: is this structural adaptation? Chronic postural loading? A healed injury from years ago? A congenital asymmetry the animal has always lived with?
This doesn’t mean assessment becomes less useful. It means the relationship between your findings and your conclusions becomes more nuanced. You move from detective work with a set of known clues to detective work where the scene has already been partially cleared. Your palpatory and observational skills matter more, not less.
Adapting the Intake Process
Before you even begin your physical assessment, your intake brief needs to flex. The standard form assumes retrospective certainty. With a rescue patient, you’re building forward from whatever the new owner can tell you, which means reframing the questions you ask.
Rather than “previous injuries,” consider asking the owner what they’ve noticed since the animal came into their care — changes in movement, posture preferences, reluctance in particular situations, reactions to touch in certain areas. This is prospective observational data, and it’s genuinely valuable. A new owner who says “she always sleeps curled to the right” or “he flinches every time someone approaches from his left side” is giving you clinical information, even if they don’t realise it.
It’s also worth asking directly what the rehoming organisation observed. Rescue centres that work closely with animals pre-adoption often notice things that don’t make it into formal documentation — a dog that won’t lie on its left hip, a horse that was difficult to catch, a cat that startles unusually at noise. These behavioural fragments can complement your physical findings considerably.
Where the history is genuinely sparse, document that clearly. “History unknown prior to rehoming” is an honest and useful notation. It tells the next practitioner reading those notes something important about the interpretive context.
What Chronic Stress Does to the Body — and Why It Matters Here
One of the most significant clinical considerations with rescue animals is the physical sequela of prolonged psychological stress. This is not a soft or speculative concept. We know that chronic fear and anxiety states create consistent muscular and postural patterns — increased flexor tone, a drawn-in posture through the trunk, altered proprioception, and heightened reactivity to touch.
A rescue dog that spent an extended period in a kennel environment, or one that experienced neglect or mistreatment, may show lumbar restriction, reduced hip extension, and sensitivity over the posterior thoracic region that has nothing to do with a discrete musculoskeletal incident. It has everything to do with how that animal held itself, day after day, month after month, in response to its emotional state.
As we’ve explored in our article on the relationship between canine emotional state and physical presentation, the fear posture in dogs — lowered hind end, tucked pelvis, rounded lumbar spine — is not just a momentary behavioural response. When sustained, it reshapes the musculoskeletal system. Hip flexors shorten. Spinal extensors become inhibited and then reactive. The quadriceps, placed on chronic stretch, become exquisitely sensitive to palpation. Fryette’s spinal laws apply whether the driving force is a physical incident or a sustained postural set.
Understanding this doesn’t change the osteopathic techniques you use, but it changes how you interpret your findings and how realistically you frame the likely course of treatment. You’re not resolving a single injury; you’re working with an adaptive system that has been recalibrated over time.
The First Session: Calibrating Your Pace
With any new patient, the first session involves reading the room. With a rescue animal, this skill becomes particularly important. You may be encountering an animal that has learned to guard, dissociate during handling, or respond to manual contact in ways shaped by experiences you know nothing about.
Recognising the communication cues your patient gives you throughout the session is non-negotiable. An animal that goes very still and flat is not necessarily relaxed — it may have learned that compliance produces less aversion. An animal that escalates quickly from curiosity to withdrawal may have a lower tolerance threshold than a dog or horse that has experienced consistent, positive handling throughout its life.
In practical terms, this means slowing down. It means giving the animal more agency in the early stages of contact — allowing it to come to you, watching for micro-signals of acceptance or avoidance, and being genuinely willing to end a session early or work only at the level the animal can comfortably tolerate. The osteopathic work will be more effective because of this patience, not in spite of it.
This is also worth communicating clearly to the owner. If you’re unable to complete a full assessment in the first session because the animal isn’t ready, that’s not a failure — it’s good clinical judgement. Setting that expectation early builds trust with the owner and prevents them from interpreting a staged approach as uncertainty or incompetence on your part.

With a rescue patient that has a layered and unknown history, it helps to think in treatment phases rather than aiming for a single-session resolution.
The first phase is principally assessment and rapport-building. You’re gathering information about the animal’s structural patterns, its tolerance of handling, and its responsiveness to gentle manual contact. You may do some light work in this phase — soft tissue, gentle articular assessment — but your primary output is a clearer clinical picture and the beginning of a working relationship with the animal.
The second phase, once the animal is more settled and you have a clearer hypothetical framework, involves working more directly with the patterns you’ve identified. This is where you begin to address compensatory loading, and restricted areas. Importantly, you’ll want to progress slowly and monitor how the animal responds between sessions. Rescue animals can show pronounced post-treatment responses — sometimes positive, sometimes involving a temporary increase in sensitivity — and owners need to know what to watch for.
The third phase is maintenance and optimisation. By this point, you should have a reasonably good understanding of what the animal’s structural baseline looks like, what patterns tend to return between sessions, and what environmental or management factors are contributing to their presentation.
Working Within the Wider Team
Rescue animals often come with a network of professionals already involved — vets, behaviourists, trainers, sometimes hydrotherapists or physiotherapists. Your role as an osteopath fits naturally into this framework, but it requires good communication in both directions.
Sharing your findings — translated thoughtfully into language that’s useful to other practitioners — contributes to a more coherent approach to that animal’s care. Receiving information from the behaviourist about how the animal is progressing socially, or from the vet about what imaging has shown, makes your osteopathic assessment more contextually informed.
It’s also worth being explicit with the owner about what osteopathy can and can’t offer in this context. You can work with physical patterns, support neuromuscular balance, and help the body adapt more comfortably as the animal’s life circumstances improve. You are not, however, a substitute for veterinary assessment, and in rescue animals with genuinely unknown histories, don’t hesitate to recommend imaging or further investigation — when the history is blank, a lower bar for referral is simply good clinical practice
Adapting Your Brief, Not Your Standards
Adjusting your brief does not mean lowering your clinical standards. It means recognising that the tools you use need to be applied with more flexibility, more interpretive humility, and more willingness to hold your hypotheses loosely until the picture becomes clearer.
Rescue animals are, in many ways, among the most rewarding patients in clinical practice. They often respond profoundly to skilled, patient manual work. The combination of structural unloading and genuine positive handling can produce changes that extend well beyond the physical — and watching that happen across a course of treatment is one of the more compelling arguments for this work.
Understanding how to approach these patients well is part of what separates a competent osteopathic practitioner from a truly skilled one. The blank spaces in the history are not a problem to solve before you begin. They are part of the clinical reality you work within — and they are navigable, if you know how to read what the body in front of you is telling you.
Imposter Syndrome in Animal Professionals: Why You Might Be Your Own Worst Enemy
By Chris Bates M.Ost DipAO
Are you an animal professional? Have you ever had that creeping feeling that you are not good enough?
Working with animals feels like a calling for many and has deep meaning for those who undertake an animal-based career. This is why it can be deeply unsettling when feelings of inadequacy crop up.
“I’m not as competent as people think.” “It’s only a matter of time until I’m found out as a fraud.”
Sound familiar? If it does, then read on and let’s investigate why.
What Is Imposter Syndrome in Animal Professionals?
It’s that internal voice that tells you, “who do you think you are?”
Imposter syndrome is irritatingly persistent, telling you that you don’t have the knowledge or the skill, or that you are falling way behind your clients’ expectations and soon you will be found out. It might make you continually second guess yourself, compare yourself to others, or try to overwork just to prove your worth to people.
The Certification Trap
Some people with imposter syndrome will chase certifications one after the other because it seems like a way to obtain validation. While doing this, they never actually commit to the principles of the certification they did to get into the career.
Obviously there is nothing wrong with gaining more knowledge — continued development is part of being an animal professional. The problem arises when it’s not done for the right reasons. When people are doing it to prove “worth” or validate themselves, this becomes a perpetual cycle of inadequacy, as there are always more certifications you can do (but should you?).
When the Most Experienced Professionals Struggle Most
Some people with imposter syndrome are ironically the most experienced and capable out there. However, they might avoid high-stakes work or even any work due to their feelings of lack. They might avoid situations where they might be put in front of other professionals for fear of being judged in comparison.
All the while, any praise from their clients can just bounce right off them rather than feed their confidence. It can feel to those with imposter syndrome like there is an invisible wall that won’t allow any positive reinforcement in.
Why Do Animal Professionals Suffer From Imposter Syndrome So Often?
The Challenge of Working With Non-Verbal Patients
The unique part of the animal industry is that animals cannot “speak” for themselves. Obviously they have plenty of other ways of communicating, but without proper knowledge of animal behaviour — which most of the general public don’t have — these communications can go misunderstood and often badly misinterpreted.
As professionals, we can spot and understand these behaviours, but owners might have a different opinion, often based on little to no credible knowledge. This discrepancy can be difficult to overcome if the owner has strongly held beliefs, even when we give a full breakdown of what we are observing and expecting.
With horse owners, it is not uncommon to hear them talk about naughty horses or blaming the horse for their behaviour. Professionally we know there is always a reason for behaviours and that they don’t suddenly just decide to be difficult. Understanding how owner perception and cognitive bias shape what clients see and believe can help you contextualise this challenge rather than internalise it as your own failure.
The Comparison Problem
Comparison is a huge problem in the animal industry. One can look at another and immediately think that they have something we don’t.
We judge ourselves on what we see elsewhere — by what other professionals are doing. Sometimes we might not even agree with the ethics, principles or methods of the other person but still somehow think that they have higher status or power than us. Social media has catapulted this problem into overdrive and many animal professionals will host large followings, making us feel further inadequacies.
Information Overload and Unrealistic Benchmarks
There is always new research and evidence in any discipline. Keeping up with the evidence and knowledge can seem overwhelming and sometimes can initiate that feeling of not being good enough. It can appear that however much you learn, you never know enough. We end up setting ourselves unrealistic benchmarks.
Difficult People in the Animal Industry
Unfortunately there are areas of the animal industry that are prone to “difficult people” showing up. This is the polite way of saying that there are those who seek to down-tread others to put themselves on a pedestal. Of course, this is a sure-fire way to reduce your self-esteem and confidence.
The horse industry is famous for people valuing opinion over evidence or education. As we all know in our current political climate, opinion can have huge power despite being wrong or cruel. In freelance work — something many of us do — travelling around to various locations, it is not unusual for another so-called “professional” to act very unprofessionally and bad mouth you or make out that you are not what that client needs.
Signs You May Have Imposter Syndrome
Do any of these sound familiar?
- You think any career advancement you get or positive outcome is more luck than judgement.
- You lose faith in your modality or techniques.
- You are burnt out, physically and emotionally.
- Obsessing over mistakes, even the most minor ones.
- Avoiding further training for fear of being “on display.”
- Anxiety and panic around even the most routine of work.
- Career stagnation — you feel like your work isn’t really going anywhere.
- Overworking to find validation, or committing to too much and then not being able to keep up, leading to eventual burnout.
- Mental health strain.

What about them indeed… Who cares? You certainly shouldn’t.
The crazy irony of this whole situation with comparison to others is that they are probably feeling the same way much of the time. If somebody puts you down, you need to question why.
The only motivations for putting someone down would be a genuine dislike of that person or feeling inadequate yourself and not having the strength to better yourself instead. People who cut you down so they appear higher are either incapable of self-reflection and betterment, or they are malicious. Either way, that actually means they are the ones who lack — not you.
So essentially there are two types of damaging characteristics: the imposter syndrome, and the opposite — the one who cuts others down due to their own sense of lack.
Giving Headspace to Those Who Deserve It
There will always be those who disagree with you. Wasting time thinking about what they think will draw you away from your actual passion, which is working with the animals. It’s unhelpful to give them space in your mind rent free.
The key to overcoming the troubling feelings is reflection — something the other people often lack. Firstly, reflect on their knowledge: do they actually know what they are talking about and do they know what you do? Next, reflect on them as a person and professional: do you like them? Do you respect them? Do they have good results? (Results, not owner opinions.)
Next, reflect on that information. If the answers were “no” to all of the above, then they deserve none of your brain power worrying. If they have something constructive to offer, then perhaps approach them to impart that information whilst ensuring they understand that talking to you first — not owners — is the professional thing to do.
There is always someone who has more experience, knows something cool and learned a special technique. Their progress doesn’t diminish your usefulness. The value of what you provide is still there and remains unchanged. Put your thoughts into being the best version of what you are rather than obsessing that you have to “match” everyone else.
How to Overcome Imposter Syndrome as an Animal Professional
Forgive Yourself First
You must forgive yourself for feeling this way and not see it as a weakness. People with imposter syndrome, while having to suffer the bad aspects, are also more likely to be conscientious and careful. They are more likely to be aware of limitations and not put people and animals at risk. Imposter syndrome can be awful, but it can also be evidence that you are only trying to provide the best.
Keep a Record of Your Wins
It can be hugely beneficial to have a record of positives to look back on, as we often forget just how far we have come. Rather than comparing ourselves to others, we can compare ourselves to our past self and see how we have progressed.
You can keep records of your certifications and continued professional development. Keep thank you messages that clients may have given you. Make a note of the nice things said about your work in a journal. Within that journal you can also record particularly successful work — but remember that successful does not just mean one thing. Success could even be completing a day of work without the imposter syndrome creeping in. Whenever you get moments of doubt, you can go back over your records.
Don’t Identify Completely With Your Work
It’s so easy to refer to myself as “Chris the Osteopath,” for example. However, I’m also Chris the person. When we take too much of our identity from what we do for work, the imposter syndrome creeps into our personal life and affects us far deeper. It is wonderful to have a calling or a passion for your work, but you are still you beyond that.
Find a Mentor You Trust
Having another person to bounce ideas off is a massive benefit to being a professional in any industry. If you are a service provider working with animals, an experienced voice to help guide you and to offer wisdom will allow you to direct your career appropriately and also voice your own concerns.
Someone looking at you from the outside may see all the positive things that your imposter syndrome is drowning out. If you’re exploring what a structured mentored pathway looks like, understanding what a career in animal osteopathy involves can also provide a useful framework for professional identity.
Prioritise Self-Care to Prevent Burnout
Burnout is real and imposter syndrome will speed it up! The vicious cycle is that if we are feeling burnt out, the imposter syndrome is louder because our reserves are too low to overcome it. Ensure that you make self-care an important part of your life. It could be getting away from time to time, booking a massage, meeting with friends and family, or just taking time for yourself with a good book.
Keep Learning — The Right Way
This doesn’t mean keep chasing certifications. Any career improves when you realise and accept that we are always students. Continual learning can be about enhancing your understanding of your own profession, not adding continuous certifications.
When people gain certification after certification, their professional identity becomes confusing — people won’t know what they actually do and may not trust their abilities. It is great to have multiple strings to your bow if you have the energy, but try to get great at what you do before diversifying. If you keep starting new paths, you never get anywhere in any of them.
Your Work Matters
It is important to remember that people will choose to use your services because it’s you, not just because of certificates and letters after your name. Your experience is valuable and that includes everything, even before you started your animal career professionally.
If you try to be someone you are not, you will end up with clients you don’t want to work with. Be genuinely and authentically yourself and you will develop the career you want. It is always good to remain open-minded and accept constructive advice, but be conscious about who you accept that advice from.
Remember what drove you to choosing this career initially and regain that spark of passion.
You don’t need to be great to start, but you need to start to be great.
Palpation in Animal Osteopathy: The Art of Assessment by Touch
By Chris Bates M.Ost DipAO
To the untrained eye, it can appear that osteopaths have some mystical ability to understand an animal and their condition simply by laying their hands upon them. But it’s not magic — it’s palpation. Palpation is the refined art of feeling and assessing the condition of an animal by touch. Osteopaths spend entire careers refining their sense of touch, though they will have developed a strong proficiency by the time they graduate. Palpation is one of the most important hallmarks of osteopathic practice, and often stands as a clear point of distinction from other professions.
What Does Osteopathic Palpation Actually Involve?
Feeling More Than You Might Think
To feel well — we need to understand that we are not just feeling one or two things. Palpation uses the entire range of touch receptors to assess. As well as feeling for the obvious lumps and bumps, we are feeling temperature, tissue texture, mobility of joints and tissues, elasticity, and asymmetry — essentially everything.
Palpation allows us to assess both the superficial and the deep. Osteopathic training gives practitioners the ability to sense the various tissues and their individual differences — from superficial palpation of the skin through to deep muscle and even viscera — allowing us to detect the state of the body as a unit.
A Practical Example: Palpating the Horse’s Hip Joint
The different tissues of the animal’s body have different properties, and when an osteopath palpates, they will detect these depending on where they are working and what tissues lie beneath their hand.
When palpating over the hip joint of a horse, for example, we can begin lightly and detect the temperature of the skin, the state of the coat, and any abnormalities such as dryness or damaged skin. Then we can feel the taut fascial connective tissue over the hip joint — quite different from other areas where fascia may be more mobile and elastic. There will be muscle and tendon tissue, each with different states of tension and elasticity. We can then palpate the joint borders and bone surfaces, including the synovial capsule and surrounding ligaments.
This all takes practice, of course, and osteopaths continue to refine this skill throughout their career.
How Does Palpation Work? The Science of Touch
Our hands are incredibly sensitive tools. Not only do we have remarkable dexterity, but the shape and structure of our hands and digits provides extraordinary perception and control. As our ancestors evolved and became less reliant on front limbs for locomotion, those limbs were freed for more advanced manipulation — a generalised specialism unlike anything seen in our ape cousins.
The Receptors Behind the Skill
The surfaces of our hands — particularly the fingers — are highly innervated with receptors that relay information to the spinal cord and brain:
- Mechanoreceptors detect pressure and movement
- Merkel cells provide perception of fine surface detail
- Pacinian corpuscles register vibration
These different receptor types send information via specific spinal tracts to the somatosensory cortex, where the brain processes this vast sensory data. Over time, these pathways become more refined. The more we use a skill, the better and more developed it becomes — and in osteopathy, palpation is fundamental to that development.
What About Reliability?
There are voices within the health and veterinary industries that question the reliability of palpation, often citing evidence of poor inter-practitioner reliability. However, this type of research fails to account for the development of skill over time and a practitioner’s varied exposure to different tissue conditions. Of course there will be variation between practitioners — this reflects the uniqueness of individuals, not a fundamental flaw in the method.
Palpation is not claimed to be infallible, nor superior to all other assessment methods. The point is that it is free, improvable, instant, and capable of clarifying the full picture of the animal in front of us.
Why Does Palpation Matter for Animal Health?
Detecting Change Before Dysfunction Appears
Osteopaths can detect subtle changes that may occur before an animal begins to display overt signs of dysfunction — leading to improved welfare and more proactive health maintenance. Osteopathic concepts like the Involuntary Mechanism (IVM), often referred to as cranial osteopathy, use palpation continually to assess changes as they occur, requiring well-honed skills to interpret.
The underlying causes of a condition can often be addressed during routine maintenance. Many animal osteopaths recommend regular check-ups to monitor these types of changes. Because animals cannot verbally describe their feelings, developing a deeper ability to detect alterations creates a more profound understanding of the animal and their health state. By building a regular connection with your animal osteopath, they can more fully understand the animal’s “normal” — and better detect when that balance has been disturbed.
Palpation as Part of a Wider Assessment
Palpation sits alongside the other assessment tools at our disposal. It is not enough on its own to form a thorough hypothesis, even in osteopathy. Active and passive assessments are vital for obtaining a holistic view — and during passive assessment, we are palpating the whole time too.
Sometimes the conclusions we move towards through observation and active assessment are contrary to what we perceive during palpation. This can create confusion, but it is a reminder that even these tools together do not provide the full picture. A thorough case history, communication with paraprofessionals, vets, and the owner are all essential. These often fill the gaps and clarify why we may palpate one thing but observe another.
Palpation During and After Treatment
One of the great advantages of developing strong palpation is the ability to reassess immediately after treatment. When we can perceive a tissue change once treatment has been applied, there is a strong likelihood it has had the desired effect. In fact, the real beauty of manual therapies as employed by osteopaths is that we can feel tissues react and change while treatment is taking place.
As my Osteopathy teachers would often say: “When you feel change, that’s when to stop.” It is very easy to overtreat an animal, and this can be just as damaging as leaving a dysfunction to perpetuate. Palpating well and sensing change in real time means we can apply only what intervention is needed to allow the body to adjust — then stop.

How to Improve Your Palpation Skills
Whether you are an animal osteopath, a different type of therapist, or a conscientious owner who wants to better connect with your animals, developing your palpation will be genuinely valuable. Here are the key pointers:
Learn the Anatomy
Understanding anatomy gives you a three-dimensional visualisation when you place your hands on the body. Professionals should always be reflecting on and updating their anatomy knowledge — but owners can benefit from this too. There are excellent books on equine and canine anatomy that make what can seem a daunting subject approachable. Contact LCAO to discuss our reading list. Speak with your vet when they visit. Practice labelling printed diagrams — or even your animals, if they are willing. Knowing muscle locations, joint structures, tendons, ligaments, and visceral positions makes you a far better perceiver of issues when they arise.
Palpate Different Animals
If you have access to a variety of animals, palpate them all — with permission — and feel the variations from species to species, breed to breed, and individual to individual. Try palpating the same area on two different horses: can you feel the differences in muscle development?
Practice Light, Medium, and Deep Pressure
By varying the level of your palpation, you will perceive different layers of tissue and densities. Start very lightly. Pressure should never blindly push through — it should be graduated and constantly responsive. Too much pressure can also alter how your receptors function, potentially numbing you to certain sensations.
Slow Down
Many people try to go too fast and miss a great deal. Imagine “melting” into the animal’s tissues and visualising the anatomy as you go. Slow is not inefficient — it is comprehensive and good practice.
Monitor the Animal’s Reactions
Palpation also includes the reactive behaviours shown when a certain area or depth is contacted. You may not feel a difference, but the animal might. Reading behaviour during palpation is an integral part of the osteopathic assessment process — particularly in dogs and other animals with complex emotional responses. Be aware that palpation is about reading the whole animal, not just the tissues.
Practice Pattern Recognition
Hold a handful of coins in your closed hand and try to differentiate them without looking. If you have the opportunity to palpate an injury or dysfunction, do so — it will help you recognise that sensation and that pattern in the future.
Get Supervision
If an experienced practitioner or osteopath can observe your technique and give feedback, this is invaluable. Compare what you feel to their conclusions, ask their opinions, observe how they approach palpation, and try to incorporate what you learn into your own style.
Conclusion
Learning palpation is a fundamental skill in animal osteopathy — and one that extends its value beyond the clinic. It teaches patience, awareness, mindfulness, and a commitment to self-improvement. Your hands are remarkable tools. Enhanced palpation skills may even help you better experience the world around you, or recognise changes in the health of those close to you.
Try out the pointers above and discover what your hands can tell you.
Navicular Syndrome in Horses: Whole-Horse Care
Navicular syndrome remains one of the most challenging and emotionally draining diagnoses in equine medicine. For decades, it has frustrated veterinarians, farriers, therapists, and owners alike — not because it is rare, but because it is complex, progressive, and rarely simple to manage well.
Traditionally, navicular disease treatment focused on pain control and corrective shoeing. While those remain essential, modern understanding has moved well beyond a single-structure model of disease. What we now call navicular syndrome is more accurately understood as a form of caudal heel pain syndrome — a condition involving multiple tissues, biomechanical forces, and compensatory patterns throughout the horse’s body.
Emerging clinical evidence and practical experience both point toward the same conclusion: sustainable management requires more than symptom control. It requires a coordinated, whole-horse approach that integrates veterinary care, farriery, and appropriate supportive therapies.
Understanding Navicular Syndrome: More Than Just a Bone Problem
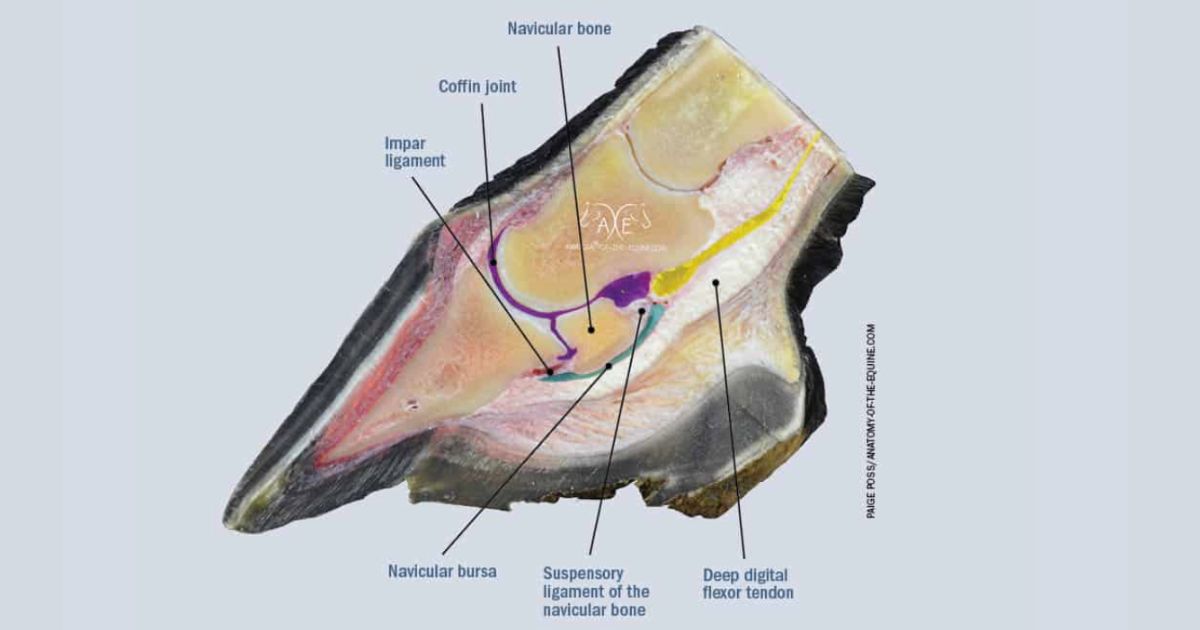
The navicular bone sits deep within the hoof, positioned between the deep digital flexor tendon (DDFT) and the coffin joint. It plays a crucial biomechanical role in force transmission, shock absorption, and movement efficiency.
However, navicular syndrome in horses is no longer viewed as isolated navicular bone degeneration. Instead, it is understood as a multifactorial condition involving a network of interconnected structures, including:
- Navicular bone remodeling and surface changes
- Deep digital flexor tendon inflammation, degeneration, or adhesions
- Navicular bursa inflammation
- Collateral sesamoidean ligament strain
- Impar ligament pathology
- Coffin joint involvement
- Altered vascular perfusion in some cases (the exact role of vascular factors remains debated)
For many horses, the disease develops gradually. Lameness is often subtle at first — intermittent, inconsistent, and easily dismissed as stiffness or training-related soreness. Over time, discomfort becomes more persistent, particularly on hard or uneven surfaces.
What makes navicular syndrome especially challenging is not just the local pathology, but the way the horse adapts. As pain develops in the caudal heel region, movement patterns change. These compensations don’t stay in the foot — they ripple through the limb, the back, and the entire musculoskeletal system.
Traditional Navicular Disease Treatment: The Foundation
Despite advances in integrative care, conventional veterinary management and corrective farriery remain the non-negotiable foundation of navicular treatment.
Veterinary Medical Management
Standard veterinary approaches typically include:
- NSAIDs as first-line pharmaceutical support to control pain and inflammation. The careful management of pain is critical, as uncontrolled discomfort leads to further biomechanical compensation and accelerated deterioration.
- Bisphosphonates (such as tiludronate and clodronate) in selected cases, where osseous pathology is evident and pain modulation is required
- Intrasynovial or intra-articular injections of corticosteroids and/or hyaluronic acid when coffin joint or navicular bursa involvement is confirmed
Historically, vasodilators such as isoxsuprine were widely used, though evidence for their effectiveness has been inconsistent and they are now less commonly relied upon in modern protocols.
Medical management plays a vital role, but it is not a cure. Its purpose is to reduce pain, slow progression where possible, and support function — not to reverse established pathology.
The Critical Role of Farriery
Corrective farriery remains the cornerstone of navicular management. The goal is biomechanical: reduce stress on the navicular region, improve breakover, optimise loading patterns, and support healthy hoof function.
Just as proper hoof care and osteopathic principles work synergistically, understanding the biomechanical implications of farriery choices helps inform the broader therapeutic strategy.
Common strategies include:
- Egg bar or heart bar shoes for heel support and load redistribution
- Wedge pads or raised heels to reduce DDFT tension
- Rolled or rockered toes to ease breakover
- Wide-web shoes for increased support
- Carefully managed barefoot protocols in select, appropriate cases
Effective navicular management requires active collaboration between vet and farrier, with regular reassessment and adjustment as the horse’s response evolves.

The Biomechanical Cascade: Why Navicular Syndrome Affects the Whole Horse
A horse with caudal heel pain doesn’t just have a sore foot — it has a changed movement strategy.
To avoid discomfort, the horse alters stride length, loading patterns, and limb timing. These adaptations create secondary stress throughout the musculoskeletal system:
- Altered loading travels up the limb, affecting joints, tendons, and ligaments
- Asymmetry develops between limbs
- Diagonal loading patterns increase strain on compensating limbs
- Back muscles adapt to uneven propulsion
- Thoracolumbar and cervical tension patterns develop
Over time, these compensations can become sources of pain in their own right. Back soreness, pelvic tension, neck stiffness, and secondary limb issues are not “separate problems” — they are often downstream effects of the primary pathology.
This is why treating only the foot often produces incomplete results.
Beyond Traditional Treatment: Integrating Complementary Approaches
Conventional treatment remains essential. But addressing the secondary biomechanical consequences of navicular pain can significantly influence long-term comfort and function.
The Role of Manual Therapy in Navicular Management
Manual therapy, including osteopathy, can play a supportive role when used appropriately and ethically within a veterinary-led plan.
It does not treat the navicular pathology itself. It addresses the compensatory patterns created by it.
For navicular horses, osteopathic assessment commonly focuses on:
- Thoracolumbar restrictions
- Sacroiliac and pelvic asymmetry
- Shoulder and cervical loading patterns
- Myofascial restrictions
- Global postural balance
The goal is not cure — it is functional efficiency. By reducing compensatory strain, the horse can move more comfortably within its physical limitations.
Manual therapy should always:
- Be coordinated with veterinary care
- Support, not replace, medical management
- Work alongside farriery strategies
- Respect inflammatory and pathological boundaries
Therapeutic Exercise and Rehabilitation
Complete rest is rarely beneficial long-term. Thoughtfully structured movement supports circulation, tissue health, muscle conditioning, and joint function.
A sensible rehabilitation approach may include:
- Controlled hand-walking on appropriate surfaces
- Managed turnout
- Gradual, progressive strengthening work
- Balance and proprioceptive training
- Low-impact conditioning modalities where available
Movement is not about workload — it’s about quality, control, and consistency.
Nutritional and Metabolic Considerations
Body condition matters. Excess weight increases loading forces through the caudal heel and accelerates mechanical strain.
While equine metabolic syndrome (EMS) is not directly causative in navicular disease, systemic inflammation, insulin dysregulation, and obesity can negatively influence tissue health, recovery capacity, and overall biomechanics.
Good management focuses on:
- Maintaining optimal body condition
- Supporting metabolic health
- Preventing secondary conditions such as laminitis
- Managing inflammatory load through nutrition
The Interdisciplinary Team Approach
Successful navicular management is never the result of a single intervention.
It depends on coordinated care between:
- Veterinarian: diagnosis, imaging, medical management, monitoring
- Farrier: biomechanical correction and hoof support
- Manual therapist: management of compensatory dysfunction
- Rehabilitation specialist: structured movement planning
- Owner: daily consistency, observation, and care
No single role is more important than the others — but none can replace the foundation of veterinary diagnosis and farriery.
When to Integrate Osteopathic Care
Osteopathic care may be appropriate when:
- Compensatory gait patterns persist despite medical management
- Secondary back, neck, or limb pain develops
- Performance plateaus despite correct farriery and veterinary care
- The veterinary team recommends supportive manual therapy
- Long-term maintenance of comfort is a goal
It is not appropriate when:
- The horse is in acute pain crisis
- Veterinary diagnosis has not been established
- It is used as a substitute for medical treatment
- Active inflammation requires rest and medical care
The guiding principle is simple: manual therapy supports management — it never replaces it.
The Classical Osteopathy Perspective on Navicular Care
Classical structural osteopathy, emphasises the interconnectedness of structure and function throughout the horse’s body. This philosophy aligns particularly well with the modern understanding of navicular syndrome as a condition with whole-body biomechanical implications.
From an osteopathic perspective, the navicular horse doesn’t exist in isolation—it functions as part of an integrated system. When pathology develops in the navicular region, the body’s natural compensatory mechanisms create a cascade of adaptations that, while initially protective, eventually become dysfunctional themselves.
Osteopathic assessment for navicular horses extends beyond the symptomatic limb to evaluate:
- Pelvic symmetry and sacroiliac function
- Thoracolumbar mobility and any restrictions
- Cervical function and poll mobility
- Forelimb and hindlimb loading patterns
- Fascial continuity throughout the body
- Overall postural balance and movement quality
This comprehensive assessment helps identify not only the primary pathology but the entire pattern of adaptation the horse has developed. Treatment then addresses both the compensatory restrictions and works to optimise the body’s inherent capacity for adaptation and healing.
Prognosis and Long-Term Management
Navicular syndrome is a progressive, degenerative condition. There is no cure.
What is possible is management.
Many horses maintain comfort and quality of life for years with appropriate care. Some remain in modified work. Others require lifestyle changes and workload adjustments. Outcomes vary widely.
Prognosis depends on:
- Stage of disease at diagnosis
- Quality of management
- Consistency of care
- Owner commitment
- Individual biological variation
Honest conversations about expectations, limitations, and welfare are essential.
Conclusion: A Comprehensive Approach to Navicular Care
Navicular syndrome is not just a foot problem. It is a whole-horse condition with whole-body consequences.
Veterinary care and farriery remain the foundation. But long-term success often depends on recognising and managing the biomechanical, postural, and compensatory effects that develop alongside the primary pathology.
When professionals work together — vet, farrier, therapist, and owner — care becomes clearer, more ethical, and more effective.
Not because navicular disease can be cured.
But because horses deserve management that is intelligent, coordinated, and compassionate.
FAQs
What is navicular syndrome in horses?
Navicular syndrome refers to chronic pain in the caudal heel region involving the navicular bone and surrounding soft tissues.
Is navicular syndrome the same as caudal heel pain?
Caudal heel pain describes the clinical presentation. Navicular syndrome describes the anatomical structures involved.
Can horses with navicular syndrome stay in work?
Some horses can remain in modified work with appropriate management, veterinary care, farriery, and monitoring. Outcomes vary by case.
Animal Meridians: Energy Pathways & Fascial Therapy
By Chris Bates M.Ost, DipAO, EEBW, BHSAI
The term “meridians” is used across the therapeutic industry to describe a number of things. The interchangeable use can create confusion around what a therapist is actually doing and the models they are using to assess and treat an animal. The fact remains however that the word is very useful to describe both energetic phenomena and the anatomical pathways of certain tissues. It can be very useful as owners to understand more deeply what their therapist is referring to and this article aims to clarify what these terms and models mean.
Understanding the Body as an Integrated Whole
The body of any animal can be described from a variety of angles. Notice I didn’t say it can be “separated out” or “broken down”, this is because I’m an Osteopath and we know that separation and isolation of systems means it is no longer a “body”. The different angles one can view the body will inevitably lead to different models of health. We could think of models of health as our way into intervention; we have to start somewhere and hopefully gain a greater understanding holistically with more information.
What Does Holistic Really Mean?
The term “holistic” gets thrown around a lot in the world of health but rarely does it actually mean addressing the whole. We see myofascial therapists referring to myofascial release as holistic, but this could only be true if the entire body was muscle and fascia…
Of course this does not mean that those therapists do not think holistically, nor does it mean that the therapy is invalid. But we need to see modalities as “ways in”, not as independent. All therapies will affect the other aspects of the being because animals (and we) are integrated units, myofascial release will affect the mind, acupuncture will affect the connective tissues, it is unavoidable and of course essential.
Now that’s cleared up (well, as clear as mud for most of us), let’s discuss some of these “angles” and how they work.
The Energy Model Meridians
Traditional Chinese Medicine and Qi Flow
The concept of energy meridians can be traced back to early traditional Chinese medicine (TCM). This concept was transported around Asia and also forms the basis of the Japanese system of Shiatsu (finger pressure). This energy concept describes a universal energy and life force existing in all living beings called Qi (Chi – Chinese, Ki – Japanese).
The health of the individual depends on the optimal flow of this energy throughout the body via meridians which are described as vessels or pathways for this energy. If this flow becomes blocked, weak or even excessive, then physical and emotional effects can appear.
The 12 Meridians and Acupoints
In TCM there are 12 meridians that correlate to an organ or system plus additional meridians that have more central functions such as the “governing vessel” and “conception vessel” which run along the spine. Along these meridians are points at which one can intervene in cases of dysfunction, these are acupoints and practitioners will use needles (acupuncture) or pressure (acupressure/Shiatsu) to clear blockages and mediate flow.
Ayurvedic Nadis and Prana
There are actually many similarities in the theory of TCM meridians and the traditional Indian system of Ayurveda. In Ayurveda, the pathways of this energy are called Nadis and the energy flowing throughout is referred to as Prana. There are similarities in Ayurvedic treatments and TCM/Shiatsu however there is often more emphasis within Ayurveda on the internal systems of control such as breathing techniques (Pranayama), nutrition and how one conducts themselves.
Obviously teaching an animal a breathing technique is rather difficult, Ayurvedic principles have however been applied to the animal model and specific modalities created. It could be argued that one could observe dysfunctional breathing patterns in an animal who is experiencing energetic dysfunction though. We must remember that a model is not just for intervention techniques but how we assess and examine, an “angle” to see from.
The Connection Between Energy Pathways and Anatomy
Although the principles of energy meridians are different to the biomechanical models, some of the energy pathways do seem to follow the path of major blood and lymphatic vessels or nerves. Some meridians being closely correlated with neurovascular bundles showing there could be a connection to their function.
As discussed, the body cannot be broken down and separated or it is no longer a body, so it comes as no surprise that this is the case because one approach will influence other systems. If we widen our lens viewing the energy meridians, we see that there is also some correlation with connective tissue pathways such as fascial lines. This is not an attempt to “explain away” the energetic principles as phenomena of the anatomy, but rather a way to highlight the validity of the approach.
Why Energy Meridians Work Well for Animals
When we look at how the intervention at meridians is aimed we can see the usefulness in animal practice clearly. Acupressure and acupuncture both deal with meridians but trying to address the entire system by the effects on just the energy system.
In TCM and Shiatsu, imbalance and poor flow of energy can lead to behavioural changes and emotional issues, with animals this can be particularly useful as an approach as unlike humans, they cannot receive talking therapies or coaching to overcome these states. Again, we have a “way in”.
Animals are particularly sensitive to touch and movement being that these are communication tools of the highest order in their evolution. The somewhat more subtle and less assertive methods of energy intervention can be a more suitable way to deal with animals who do not tolerate harder touch or too much contact.

Fascial Lines
What are Fascial Meridians?
Sometimes described as fascial meridians, the lines that appear in the fascial connective tissue in animals play a different role to the energy lines. The fascia is a collagen rich connective tissue which wraps and binds pretty much everything else in the body.
It plays a number of roles such as support, communication of forces, fluid transfer and it is even piezoelectric contributing to signaling. Our quadruped animals need to distribute their weight differently to ourselves as bipeds. This is why although there are many similarities with human fascia, animals rely on different fascial meridian layouts.
Understanding Fascia in Practice
Many will have seen fascia if you have bought meat from the butcher and seen the silvery/white covering of connective tissue and you will have felt it if you have placed your hand on a horse’s twitching shoulder. Although there seemed within the therapist community to be a push towards making out that fascia was some kind of newly discovered “holy grail” in healing, the reality is that this is not new and fascia has always been impacted by the approaches of manual and physical therapists.
Of course our understanding of fascia has improved with research and this serves to allow us a clearer understanding around why our approaches work so well.
Key Fascial Lines in Animals
If one were to look at a map of fascial lines annotated onto a picture of a horse or dog, they would not look too dissimilar to some of the energy diagrams. But this model uses tracking of fascial forces and tensions. This is again just another “way in” to the whole.
The Superficial Dorsal Line (SDL)
One fascial pathway often referred to within manual therapy is the superficial dorsal line or SDL. This line tracks from the occiput (caudal skull), along the dorsal aspect, down the caudal aspect of the hind limb and into the plantar fascia. The SDL aids in the stored force required for propulsion and elasticity in that movement and also supports posture, blending with very strong structures like the nuchal ligament and supraspinous ligament.
Dysfunction in this SDL can lead to lack of hind end engagement, reluctance in spinal extension and postural impacts.
Frontal and Spiral Lines
Conversely there are frontal or core lines and the superficial ventral line that support truncal flexion, breathing, digestive function and assist in guarding and anxiety related behaviours. The spiral lines assist in torque required for rotational movement and complex body movement coordination, dysfunction here can show in lateral asymmetries (static and dynamic) and difficulty in tight turns.
Signs of Fascial Disruption
It’s clear to see there are a diverse range of signs and symptoms that can be observed in fascial disruption. When one considers that fascia not only follows lines of force through the musculoskeletal system but also interconnects with the viscera, vessels and nerves, it becomes apparent to us that there are far reaching systemic effects of fascial disruption too.
How is Fascia Treated?
So how is it treated? Fascia responds well to light sustained touch when tethering or restriction are present. Slower movements and gliding touch can encourage layers of the fascia to slide and alter the friction coefficient by influencing the distribution of hyaluronic acid (the lubricating gel-like substance found within fascial tissue).
Therapists also claim that myofascial strokes improve hydration of the fascia in general but this claim is less researched; Osteopathically it does make sense as improving motility and vascular perfusion should allow for fluid transfer changes. These slower movements and softer touch do seem to have positive influences however, are these purely due to fascial “unwinding” and stretching? Osteopathy would argue, No…
The Osteopathic Perspective of Both Meridian Models
Using Different “Ways In” to See the Whole
As is repeated throughout this article, we are using “ways in” to the whole. When eating a meal, we don’t just engulf the whole thing in one go or we choke. We take smaller bites until we have the entire thing digested. This is how the picture of an animal’s health appears to us.
In Osteopathy we want to obtain a picture of the whole animal and their complaint. Do we look at the biodynamics or the behaviours? Do we look at the posture or the pain? The answer of course is that we need to look at all of those but we need to metaphorically “move around” to see all those angles.
The Osteopathic Assessment Approach
Within that “moving around” we will use assessment tools such as fascial lines, dynamic assessments and indeed we may look at energy meridians (if we have training in that area). Osteopathy is not so much about trying to eat the metaphorical meal in one bite, it’s about understanding there is a whole meal. By understanding the unity of all the systems and structures, we know that our hypothesis will only be a guide to what is actually happening.
Benefits of the Energy Model in Osteopathy
Energy work and Qi/Prana flow are an intriguing way to see the body and there are some benefits to observing from this traditional medicine approach. One plus to this model is that a meridian that is located in one part of the body will influence systems away from that location. Rather than simply accepting that as the way it is, in Osteopathy we can ask “why?” and investigate the interconnectedness through all the potential pathways.
Another plus is that energy work seeks to remove blockages and barriers to flow, this is exactly what Osteopathy does too. Rather than putting in something seen as missing or extracting an illness as if it were an entity on its own, Energy work promotes the animal’s own intrinsic healing mechanisms.
How Fascial Lines Inform Osteopathic Practice
Fascial lines/meridians show us as Osteopaths another tissue that could be affected by trauma or systemic imbalance/allostasis. Osteopathy has always been about deeply understanding anatomy. The better our knowledge of anatomy, the more we can hypothesise where health may be hindered.
Fascia feeds perfectly into our concept of bio-tensegrity, it offers Osteopaths another avenue beyond muscle connection, tendon and ligament to visualise forces being transmitted throughout the body.
Explaining Connections to Owners and Vets
Osteopathy used the term somatic dysfunction and models such as somatovisceral and viscerosomatic reflexes to explain certain presentations; Fascia offers an explanation for the connections that may (without it) seem tenuous and difficult to rationalise with owners and Vets.
Osteopathy remains open to new discoveries and to the traditional approaches alike. This is a strength in practice by not becoming biased to one model.